Age-related macular degeneration (AMD) is the leading cause of irreversible central vision loss in adults over 50. By 2050, the American Academy of Ophthalmology projects nearly 22 million Americans will be living with the disease (1). The dry form makes up around 80% of cases. For decades, the only options have been AREDS2 supplements, dietary changes, and regular monitoring (2). That gap explains why LED light therapy for macular degeneration now comes up so often in clinical practice. The real question is simple. Does the science back it up, or do red light therapy lamps macular degeneration claims belong outside evidence-based ophthalmology?
Published on April 20, 2026
LED Light Therapy for Macular Degeneration: Does It Really Work?
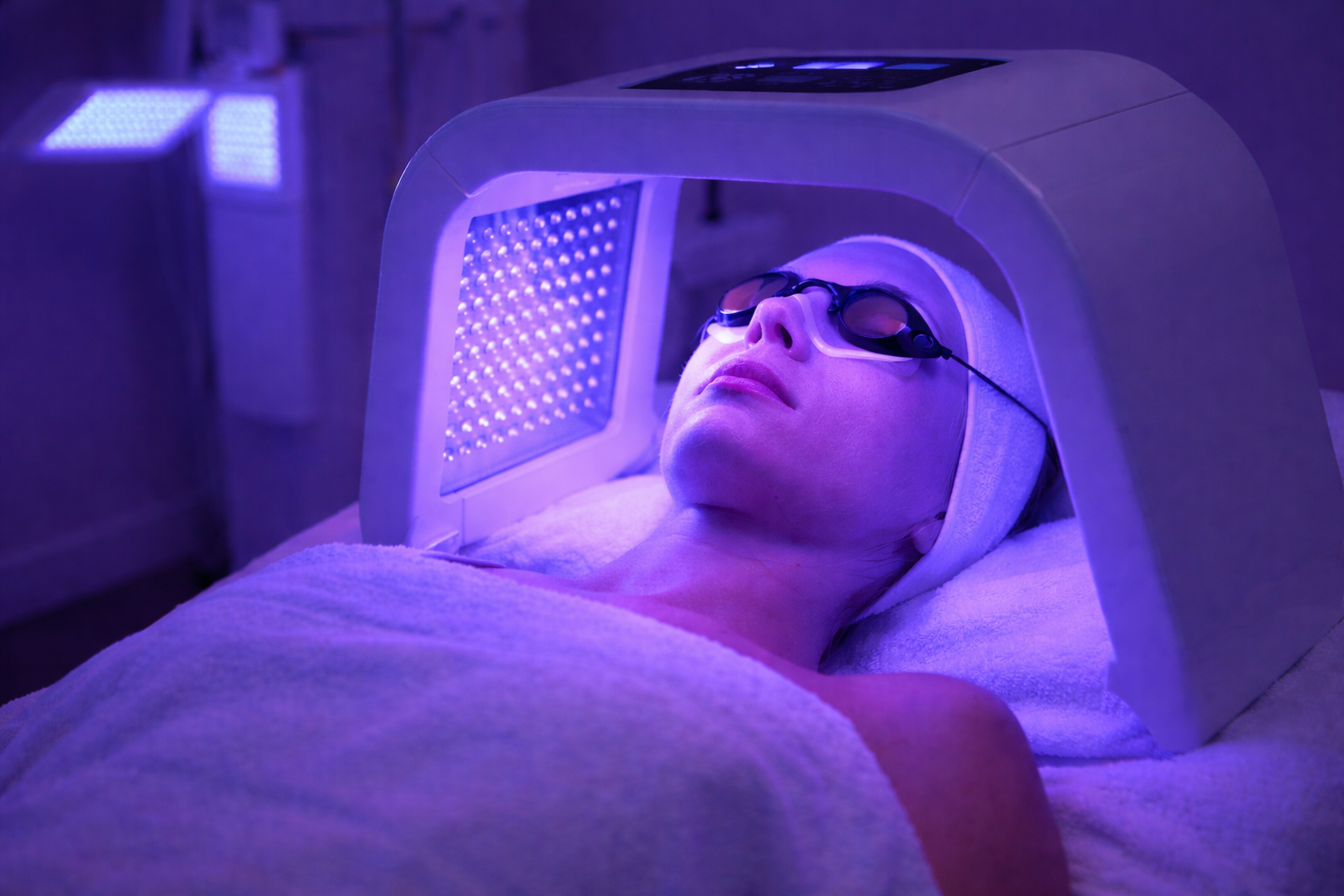
What Is Macular Degeneration
AMD is a progressive disease of the macula, the small central area of the retina responsible for sharp, detailed vision used in reading, driving, and face recognition (2). Macular damage produces blurred or distorted central vision, while peripheral sight is generally preserved – patients often describe being able to see the rim of a clock but not its hands.
The disease presents in two clinical forms. Dry (non-exudative) AMD accounts for approximately 80–90% of diagnoses and is characterised by gradual thinning of the macula together with the accumulation of yellow sub-retinal deposits called drusen (2,3). Wet (neovascular) AMD is less frequent but considerably more aggressive, driven by abnormal choroidal blood vessels that leak fluid and blood under the retina. Although wet AMD represents only about 10% of cases, it is responsible for the majority of severe legal blindness attributable to the disease (3). All wet AMD begins as dry disease, and a subset of dry AMD eventually progresses to geographic atrophy – an advanced form affecting an estimated five million people worldwide (3).
What Is LED Lamp Therapy and How It Works
In clinical literature, LED light therapy is called photobiomodulation, or PBM. The older term is low-level light therapy. The technology uses non-thermal red and near-infrared light, typically 600 to 1100 nm, delivered through LEDs or low-power lasers (5). This is a separate modality from the ultraviolet phototherapy used in dermatology – the topic of our Benefits Narrowband UVB Therapy overview. PBM wavelengths do not damage DNA. They do not heat tissue.
The biology centres on one enzyme: cytochrome c oxidase, complex IV of the mitochondrial respiratory chain. Its copper and heme centres absorb red and near-infrared wavelength 670 nm efficiently (5). Photon absorption sets off a defined cascade. Inhibitory nitric oxide releases from its binding site. Electron transport accelerates. Mitochondrial membrane potential climbs. ATP output rises (5). After that come the secondary effects – shifts in reactive oxygen species, calcium signalling, and transcription factors that activate antioxidant and anti-inflammatory pathways (5,6).
The retinal relevance is straightforward. Photoreceptors are some of the most metabolically active cells in the body. Per gram, they consume more oxygen than any other tissue. They are densely packed with mitochondria for that reason (5). Mitochondrial decline is one of the earliest cellular changes in macular ageing. That makes the retina a logical target for infrared light therapy eye research.
Can LED Light Therapy Help with Macular Degeneration
The clinical rationale of photobiomodulation AMD treatment follows directly from the cellular mechanism. Restoring mitochondrial efficiency in stressed retinal cells mitochondria may support photoreceptor and retinal pigment epithelial (RPE) function. It may also reduce the chronic low-grade inflammation behind drusen formation and slow the slide toward geographic atrophy (6). Animal data back this up. In aged mice and complement factor H knockout models – the standard AMD analogue – brief 670 nm exposure upregulates cytochrome c oxidase. It lowers complement C3. It reduces inflammatory markers in the retina (6).
Translating this into measurable patient benefit is another matter. Several early-phase studies report modest visual acuity improvement, gains in contrast sensitivity, and imaging-based drusen reduction after PBM (4,11). The findings warrant cautious optimism. They do not justify firm conclusions.
For clinics looking to broaden their therapeutic offerings beyond UV-based modalities, our catalogue covers a range of professional phototherapy systems. For wider integration into clinical practice, see our guide on Expanding Clinic Services with Multi-Indication Phototherapy.
What Does Research Say
The strongest clinical evidence comes from one programme: LIGHTSITE. It evaluated the LumiThera Valeda Light Delivery System – a multiwavelength device using 590, 660, and 850 nm light. LIGHTSITE III was the pivotal trial. Randomised. Sham-controlled. 100 patients, 148 eyes, all with intermediate dry AMD. The protocol: nine sessions over three to five weeks, repeated every four months for two years (4). At thirteen months, treated eyes gained an average of 5.4 letters of best-corrected visual acuity. The sham group gained 3.0. The difference was statistically significant (4). Around 55% of treated eyes picked up at least five letters. New geographic atrophy occurred in 1.1% of PBM eyes versus 9.8% in sham (4). On the basis of these data, the FDA cleared Valeda in November 2024 as the first non-invasive treatment for early and intermediate dry AMD in the United States (1,9).
The wider evidence base is less clear-cut. A 2024 systematic review and meta-analysis pooled three randomised trials across 247 eyes. It confirmed a statistically significant BCVA gain of about 1.76 letters and a small drusen reduction. But the trial sequential analysis was unambiguous: the required information size sits near 555 eyes, and the data fall well short. The evidence cannot yet be called conclusive (7). A 2025 follow-up was more sceptical. It concluded that current pooled data fall short of demonstrating clinically meaningful benefit. Larger and longer trials are needed before PBM enters standard care (8). A separate 670 nm-only pilot in intermediate AMD found nothing – no improvement in visual function, no improvement in retinal structure across twelve months (11). Wavelength combination and protocol are likely critical variables.
So does red light therapy improve vision in AMD? In some patients. In some trials. By a modest margin. And only with medical-grade multiwavelength devices delivered under ophthalmologic supervision. The EUROLIGHT observational study is now tracking 500 to 1,000 European patients across all stages of AMD. It should deliver real-world data over the next several years (10).
Safety and Who It May Help
Across the major trials, PBM has shown a favourable safety profile. No serious device-related adverse events have been reported. Only occasional transient afterimages occur immediately after treatment (1,4). One signal warrants attention. LIGHTSITE III recorded a small numerical increase in conversions to wet AMD in the treated arm – a finding that justifies ongoing surveillance in real-world practice (1).
AMD light therapy treatment with Valeda is currently indicated for patients with early to intermediate dry AMD who retain reasonable central vision. It is not appropriate for wet AMD. Nor for advanced geographic atrophy involving the fovea. Patients with photosensitivity disorders, light-triggered seizures, or recent use of photosensitising medications should be excluded. Consumer-grade red light therapy lamps macular degeneration products marketed online have not been validated for retinal use. They should not be treated as substitutes for clinically supervised therapy. Direct ocular exposure to unregulated LED sources may carry its own risks.
Patients should also understand that PBM is not curative. It is a disease-modifying option. It may slow progression and improve specific functional measures in carefully selected candidates. It does not reverse advanced damage. It must never replace standard ophthalmologic care, AREDS2 supplementation where indicated, or anti-VEGF therapy in wet disease.Selecting the right light-based approach for any individual patient – whether in ophthalmology or dermatology – depends on diagnosis, disease stage, and treatment goals, which is the broader principle we outline in our Personalized Phototherapy Guide.
In summary, LED light therapy for macular degeneration is one of the few non-invasive interventions backed by randomised evidence in dry AMD. The benefit is modest. Long-term durability is unproven. Meta-analytic data are mixed. For patients with early or intermediate disease, PBM may be a reasonable topic to discuss with a retina specialist. It is not yet routine – and certainly not a substitute for evidence-based care.
References
- American Academy of Ophthalmology. FDA Authorizes Light Therapy for Dry AMD. https://www.aao.org/eye-health/news/light-therapy-photobiomodulation-dry-amd-ga
- American Academy of Ophthalmology. Understanding Macular Degeneration. https://www.aao.org/eye-health/diseases/amd-macular-degeneration
- BrightFocus Foundation. Macular Degeneration Facts & Figures. https://www.brightfocus.org/macular/facts-figures/
- Boyer D, Hu A, Warrow D, et al. LIGHTSITE III: 13-Month Efficacy and Safety Evaluation of Multiwavelength Photobiomodulation in Nonexudative (Dry) Age-Related Macular Degeneration Using the LumiThera Valeda Light Delivery System. Retina, 2024. https://pubmed.ncbi.nlm.nih.gov/37972955/
- Frontiers in Ophthalmology. Photobiomodulation use in ophthalmology – an overview of translational research from bench to bedside, 2024. https://www.frontiersin.org/journals/ophthalmology/articles/10.3389/fopht.2024.1388602/full
- Begum R, Powner MB, Hudson N, Hogg C, Jeffery G. Treatment with 670 nm Light Up-Regulates Cytochrome C Oxidase Expression and Reduces Inflammation in an Age-Related Macular Degeneration Model. PLOS One, 2013. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0057828
- Rassi TNO, et al. Photobiomodulation efficacy in age-related macular degeneration: a systematic review and meta-analysis of randomized clinical trials. International Journal of Retina and Vitreous, 2024. https://pubmed.ncbi.nlm.nih.gov/39148091/
- Is Multiwavelength Photobiomodulation Effective and Safe for Age-Related Macular Degeneration? A Systematic Review and Meta-Analysis. Ophthalmology and Therapy, 2025. https://pmc.ncbi.nlm.nih.gov/articles/PMC12006650/
Healthline. Red Light Therapy for Macular Degeneration. https://www.healthline.com/health/eye-health/red-light-therapy-for-macular-degeneration
FAQ
-
No. PBM does not cure AMD. Available data suggest it may slow progression and modestly improve visual function in selected patients with early or intermediate dry AMD. The disease itself is not reversed (1,4).
-
Medical-grade multiwavelength systems delivered in clinical settings have shown a strong safety profile across the LIGHTSITE trials. No serious device-related adverse events were reported. Only mild, transient afterimages occurred (1,4). Consumer LED lamps have not been validated for retinal use and should not be aimed at the eyes.
-
In LIGHTSITE III, measurable BCVA improvements appeared after the first treatment series. They reached statistical significance by the thirteen-month assessment, after several repeated treatment courses (4).
-
In the multiwavelength Valeda trials, around 55% of treated eyes gained at least five ETDRS letters at thirteen months. Average gains were close to 5.4 letters (4). Pooled meta-analytic estimates are smaller - about 1.76 letters - and considered borderline in clinical significance (7,8).
-
Current evidence supports use in patients with early to intermediate dry AMD who retain reasonable central vision and have no contraindications such as photosensitivity. The decision should be made jointly with a retina specialist after a full ophthalmic evaluation (1,4).