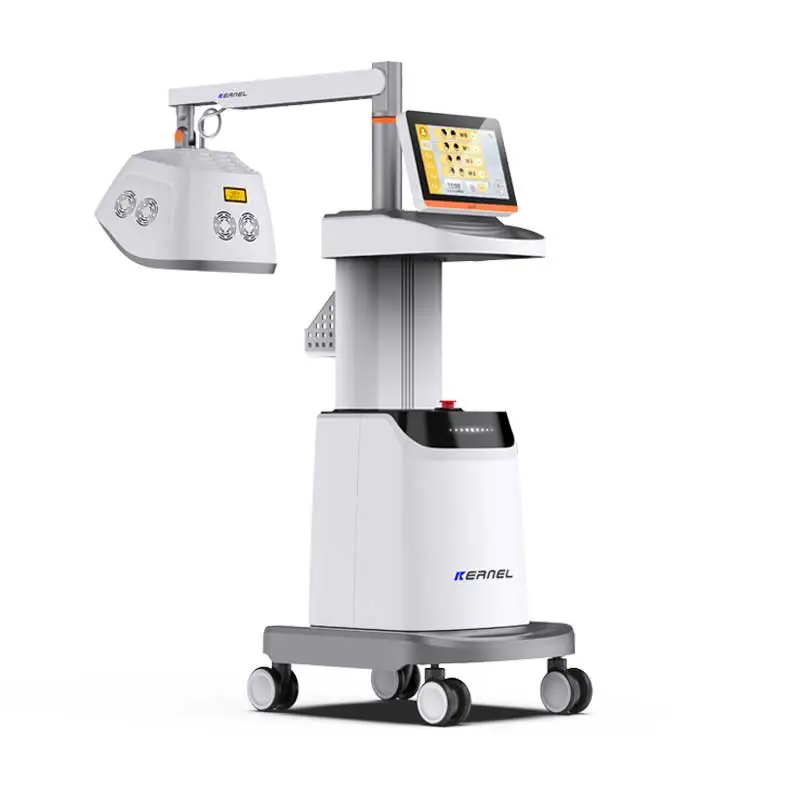
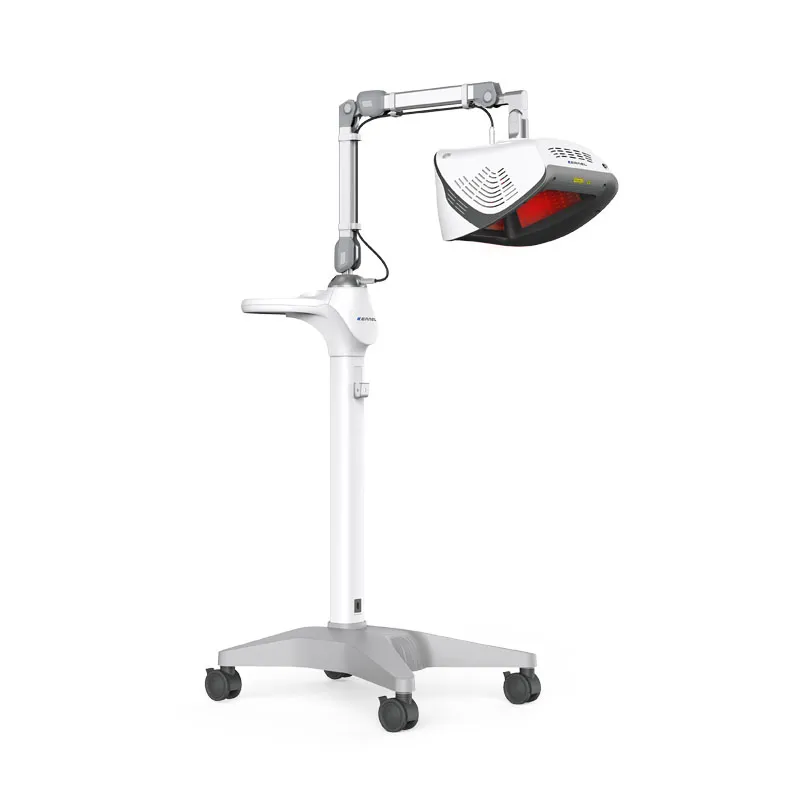
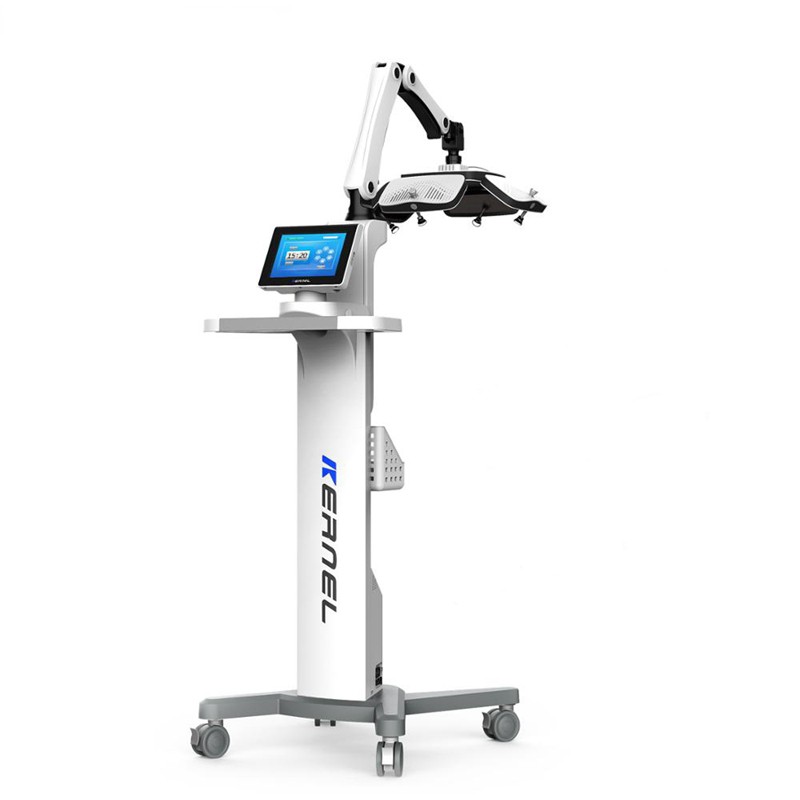
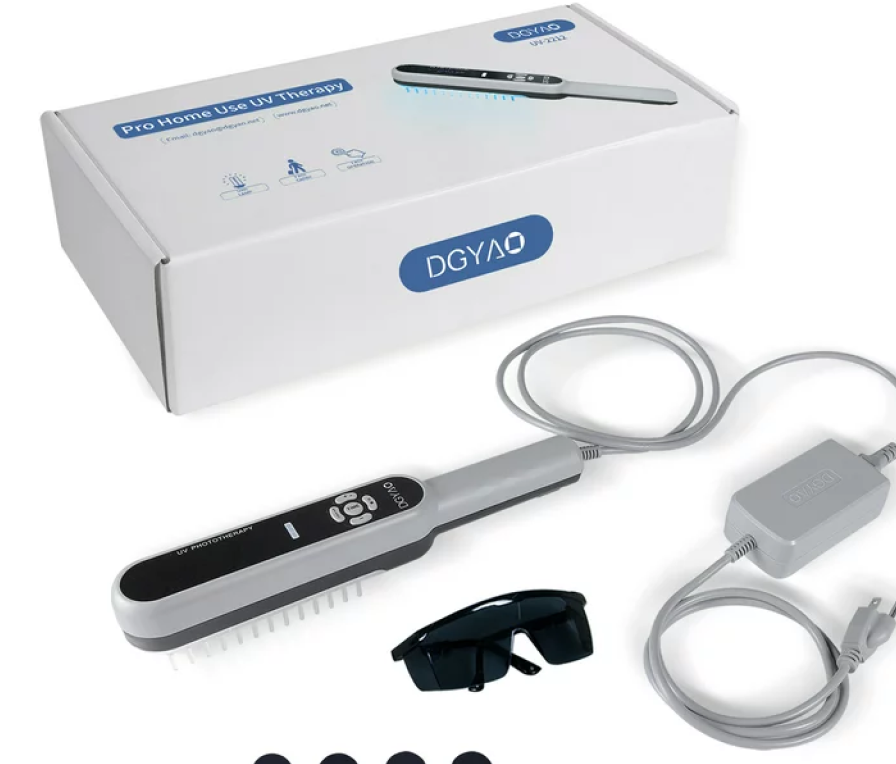
Most dermatology practices that invest in a phototherapy cabin end up using it for one or two diagnoses at most – typically plaque psoriasis and sometimes atopic dermatitis. That limited use leaves the equipment idle for hours each day and ignores a well-documented clinical reality: narrowband ultraviolet B (NB-UVB) at 311–313 nm is effective across a far wider range of inflammatory and pigmentary dermatoses (1, 2). Multi-indication phototherapy – the deliberate scheduling of one UV system across multiple diagnostic categories – allows clinics to expand services efficiently without multiplying their capital expenditure. For practices evaluating how to expand dermatology clinic services in a crowded therapeutic landscape, this remains one of the most straightforward paths forward. UVTREAT, as a distributor of professional-grade Kernel phototherapy systems, provides the equipment and protocol support that make such expansion practical.
Published on April 21, 2026
Expanding Clinic Services with Multi-Indication Phototherapy
Why Clinics Are Turning to Phototherapy
A few things have changed in recent years. Patient preference is one of them – not everyone with moderate psoriasis or eczema wants long-term immunosuppression, and younger patients in particular ask about non-invasive options before biologics come up (3). NB-UVB fits that request well. It works through apoptosis, cytokine shifts, and regulatory T-cell activity without adding anything systemic to the patient’s body (4).
The patient pool is also larger than it used to be. Psoriasis affects around 3.2% of the global population per the joint AAD–NPF estimates (5), and when you add atopic dermatitis, vitiligo, and early-stage mycosis fungoides, the number of candidates in the U.S. alone runs into the tens of millions (6). Interestingly, despite the rise of biologics, Medicare phototherapy billing grew 5% per year between 2000 and 2015 (7).
What Conditions Can Be Treated with Phototherapy
The BAD/BPG 2022 guidelines include 38 separate NB-UVB recommendations (2).
Psoriasis is still the lead indication. AAD–NPF 2019 guidelines call for NB-UVB two to three times weekly; three sessions clear plaques in a mean of 58 days versus 88 for two (5). Combined with methotrexate, clearance improves and recurrence drops (8). In half-body studies on adalimumab, the UV-treated side showed a 33% greater PASI reduction (8). These combination data matter – they make the case that phototherapy for psoriasis and biologics are not an either/or choice.
Atopic dermatitis is next. The 2023 AAD guidelines give a conditional recommendation for NB-UVB in adults with topical-refractory disease, based on a Cochrane review of 32 trials and 1,219 patients (3). UK NICE guidance extends this to children as second-line therapy (2), which is relevant for practitioners who also treat pediatric dermatology populations.
Vitiligo courses run longer – often 200+ sessions – but the evidence holds. In May 2025, the CPT revision extended excimer laser coverage well beyond psoriasis, now covering vitiligo, AD, MF, lichen planus, alopecia areata, and CTCL. That change brought roughly 20 million additional patients into the reimbursable pool (6).
NB-UVB has documented efficacy in morphoea, pityriasis lichenoides (one study showed 88% complete remission), chronic urticaria, prurigo nodularis, granuloma annulare, and photodermatoses (1, 2, 9). Diagnostic accuracy matters here – clinicians who see overlapping presentations, for instance scaly plaques that could be psoriasis vs fungal infection, need to rule out infection before starting UV therapy. The clinical takeaway is straightforward: one platform, several protocols, many treatment pathways.
How Multi-Indication Phototherapy Expands Services
Patient volume rises because referrals that used to be redirected can now be accepted in-house. A cabin running only psoriasis sessions may be busy three hours a day; the same cabin treating psoriasis, eczema, vitiligo, lichen planus, and early MF runs substantially fuller without any new hardware.
Service range widens at low incremental cost. Treating additional UV-responsive conditions requires protocol changes – starting doses, escalation rates, session frequency – not new equipment. Staff trained on dosimetry and Fitzpatrick typing apply those skills across every indication, which is why phototherapy for psoriasis eczema vitiligo and other skin conditions is one of the most capital-efficient expansions in medical dermatology.
Equipment efficiency improves in parallel. The North American phototherapy equipment market is projected near $80.9 million in 2025, with the home segment growing at 8.2% CAGR (10). Clinics using their UV therapy equipment across the full range of indications recover capital faster and lower per-session cost.
The broader clinical value of adding phototherapy is reinforced by cost data. McCoy et al. (2023) found NB-UVB the most cost-effective psoriasis therapy at $1,714/month per PASI 75, against $2,076–$2,502 for the cheapest biologic (11). BAD notes a UK NB-UVB course at £300–400 – roughly 10–30 times less than a year of biologic therapy (2).
What Clinics Should Consider Before Adding Phototherapy
Proper UV therapy clinic setup is not optional. Four things need attention before the first patient.
Equipment selection drives what you can treat. Full-body NB-UVB cabins cover the widest range, while targeted panel or handheld devices are better for scalp psoriasis or palmoplantar disease. UVTREAT’s Kernel line includes cabin, panel, and handheld options designed around consistent protocols.
Staff training goes beyond the control panel. Nurses and technicians need to understand MED determination, dose escalation, erythema grading, and HSV reactivation risk (2). StatPearls guidance adds that staff entering an active cabinet should wear UV goggles, face shields, and SPF >30 sunscreen (4).
Treatment protocols have to be condition-specific. Psoriasis and eczema protocols differ in starting dose and escalation; vitiligo runs much longer. Written protocols referenced to current AAD and BAD publications are the baseline standard.
Safety requirements include UV eyewear, genital shielding, pregnancy screening with 0.8 mg daily folate supplementation (5), cumulative dose tracking, and routine lamp calibration. Underdosing wastes the patient’s time; overdosing creates burn and carcinogenesis risk.
From Clinic to Home Use: Extending Patient Care
Access is the biggest barrier to phototherapy adherence. The LITE study – a 2024 PCORI-funded randomized trial of 783 patients across 42 U.S. sites – found home NB-UVB non-inferior to office treatment in all skin types, with adherence at 51% versus 16% and no discontinuations for adverse events in either arm (12). For dermatology phototherapy clinic services, this is significant: treatment does not have to stop when a patient’s schedule or location makes in-office visits impractical.
UVTREAT works on both sides of this equation, supplying clinics (B2B) and supervised home-use devices (B2C). The practice keeps the patient and bills for ongoing management; the patient keeps receiving treatment. Given that 89% of U.S. counties have no phototherapy facility (8), home-use is often the only way sustained treatment happens at all.
Conclusion
Multi-indication phototherapy lets dermatology practices treat more patients across more diagnoses using equipment that is relatively modest in cost next to other capital investments. The evidence – from AAD and BAD guidelines through JAMA Dermatology cost analyses – supports phototherapy as safe, effective, and financially sensible. Combined with home-use programs and proper staff training, it scales well for both the practice and the patient.
References
- Branisteanu D, Dirzu D, Toader M, et al. Phototherapy in dermatological maladies (Review). Exp Ther Med.
- Goulden V, et al. British Association of Dermatologists and British Photodermatology Group guidelines for narrowband ultraviolet B phototherapy 2022. Br J Dermatol.
- Davis DMR, et al. Guidelines of care for the management of atopic dermatitis in adults with phototherapy and systemic therapies. J Am Acad Dermatol
- Phototherapy. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing;
- Elmets CA, Lim HW, Stoff B, et al. Joint AAD–NPF guidelines of care for the management and treatment of psoriasis with phototherapy. J Am Acad Dermatol.
- STRATA Skin Sciences. AMA CPT Editorial Panel accepts revision to CPT codes 96920–96922 for excimer laser. May 2025. Reported via The Dermatology Digest.
- Mostaghimi A, et al. Trends in phototherapy utilization among Medicare beneficiaries in the United States, 2000 to 2015. J Am Acad Dermatol.
- Torres AE, Lyons AB, Hamzavi IH, Lim HW. Role of phototherapy in the era of biologics. J Am Acad Dermatol.
- Myers E, Kheradmand S, Miller R. An update on narrowband ultraviolet B therapy for the treatment of skin diseases. Cureus.
- Fortune Business Insights. Phototherapy Equipment Market Size, Share & Industry Analysis. Report, 2026.
- McCoy J, et al. Systematic review and estimated cost-efficacy of biologics compared with narrowband ultraviolet B light for the treatment of moderate to severe psoriasis and atopic dermatitis. Int J Dermatol.
- Gelfand JM, Callis Duffin K, et al. LITE Study: Light Treatment Effectiveness – home versus office NB-UVB for psoriasis. Published in JAMA Dermatology, 2024. Reported via the National Psoriasis Foundation.
FAQ
-
In simple terms, it means using the same UV cabin or panel for several different skin diseases rather than just one. The wavelength stays the same - NB-UVB at 311–313 nm - but the treatment protocol shifts based on diagnosis. Psoriasis, eczema, vitiligo, lichen planus, and mycosis fungoides each have their own dosing schedule. The hardware does not change between patients; the clinical protocol does. That is what makes this model practical for busy practices.
-
The BAD/BPG 2022 guidelines list 38 NB-UVB recommendations (2). Daily practice centers on psoriasis, atopic dermatitis, and vitiligo, but the evidence reaches further - morphoea, pityriasis lichenoides, early MF, prurigo nodularis, chronic urticaria, granuloma annulare, and a number of photodermatoses. CPT reimbursement for excimer laser was also widened in May 2025 to include vitiligo, AD, MF, lichen planus, alopecia areata, and CTCL (6).
-
In most cases, yes. Treatment courses span months with two to three weekly visits, producing a steady billing rhythm that many procedural services lack. McCoy et al. (2023) calculated an adjusted cost of $1,714 per PASI 75 for NB-UVB versus $2,076–$2,502 for the cheapest biologic (11). Lamp life runs into thousands of hours, and one trained team handles every indication - so shifting from a single-diagnosis schedule to a multi-diagnosis one fills open slots and improves margin without additional capital.
-
Start with the right equipment. A full-body NB-UVB cabin covers the most diagnoses, though targeted devices help for scalp psoriasis or palmoplantar vitiligo. Staff training comes next - not just button-pressing but MED testing, Fitzpatrick typing, dose escalation, and recognizing erythema and HSV reactivation early. Every condition treated needs a written protocol from current AAD or BAD guidance. Safety logistics - UV goggles, genital shielding, cumulative dose records, scheduled lamp calibration - close the loop. UVTREAT assists practices through this with Kernel equipment selection and technical support.