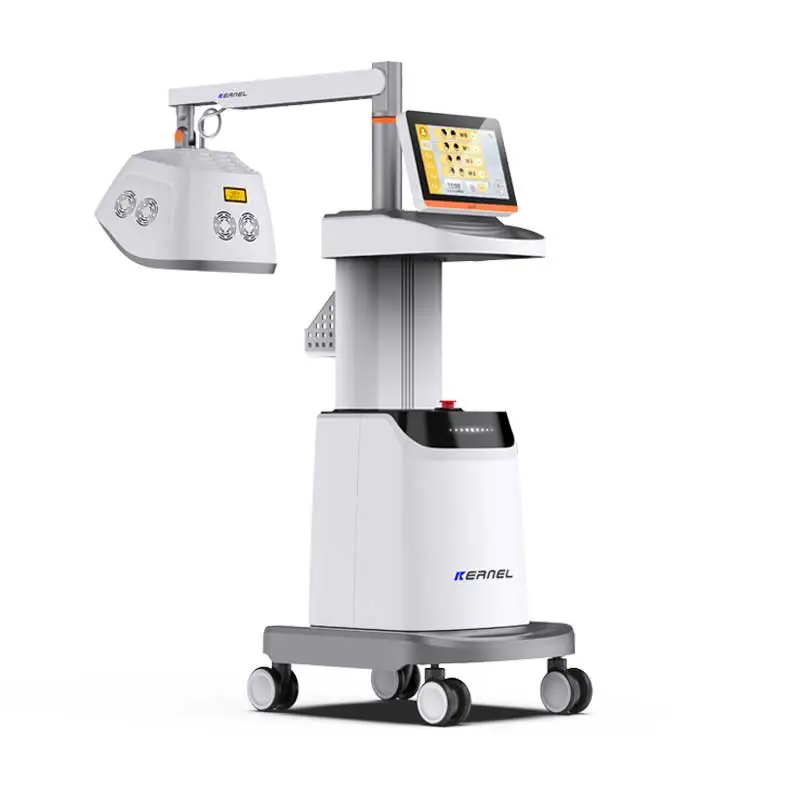
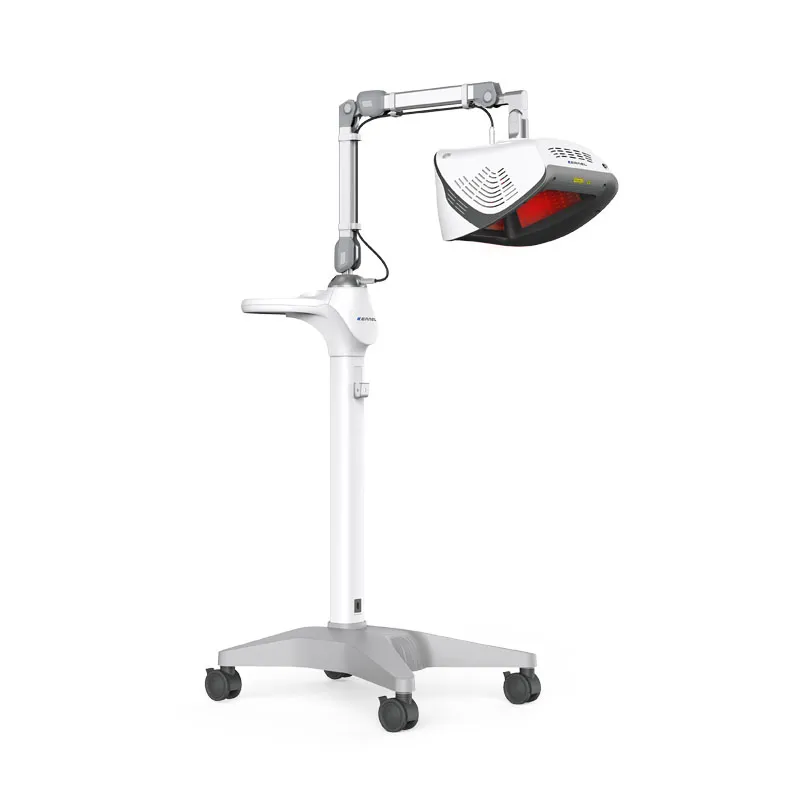
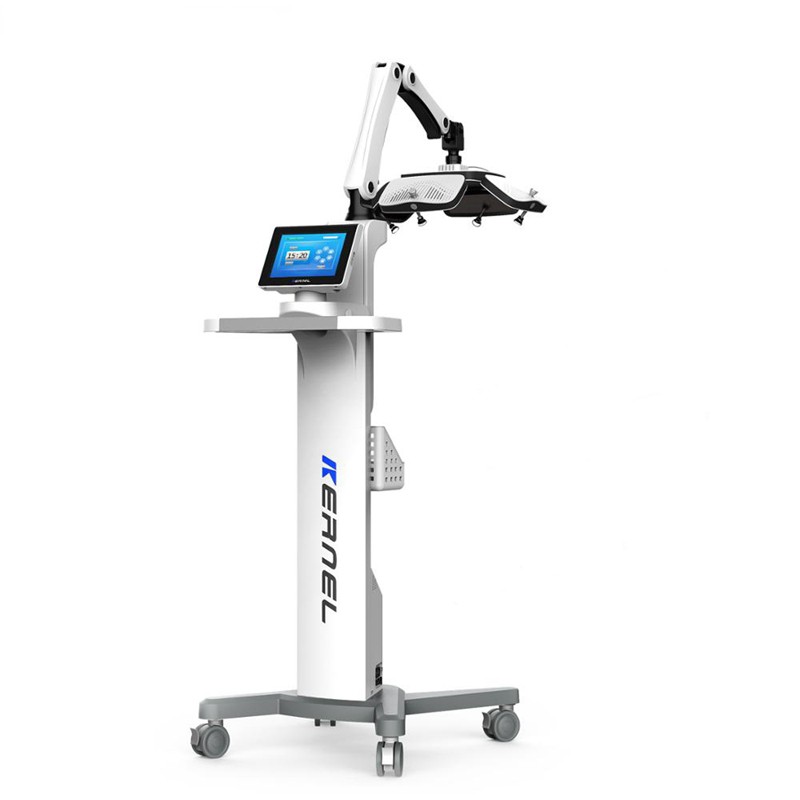
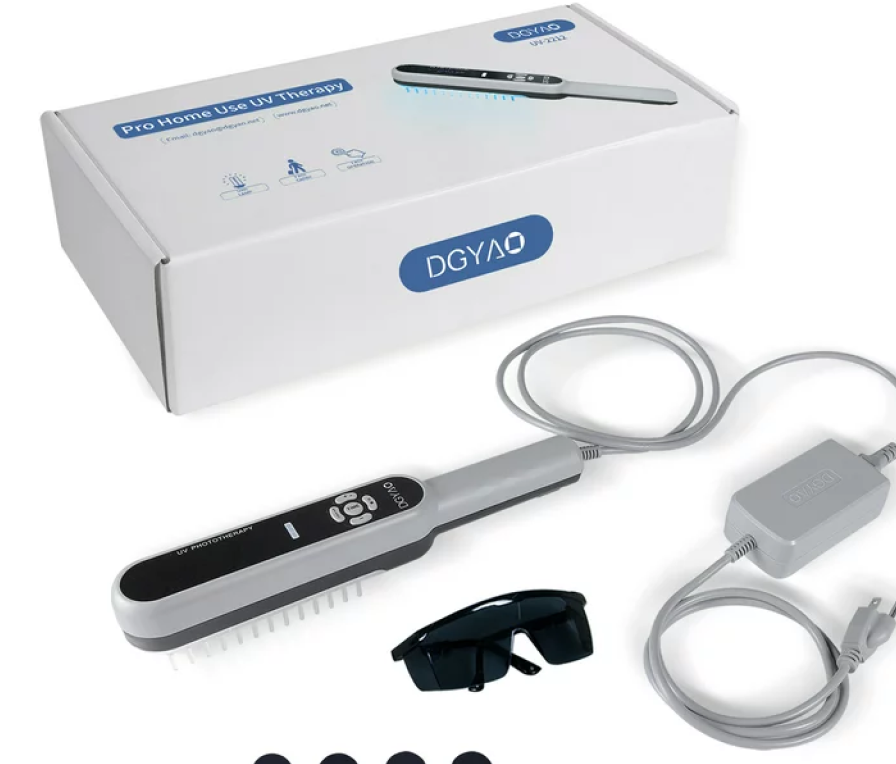
Selecting between phototherapy and biologic therapy is a common decision point in the management of psoriasis, atopic dermatitis, and vitiligo. Both options deliver real clinical results. But the cost of phototherapy vs biologics tells a very different story depending on whether you look at it from the patient side, the clinic side, or the payer side. This piece breaks down the numbers, the evidence, and the practical trade-offs – and explains where UVTREAT equipment fits into the picture for practices and patients looking for a cost-effective path forward.
Published on April 21, 2026
Cost Comparison: Phototherapy vs Biologic Treatments
How Phototherapy and Biologics Differ
In phototherapy, affected skin is exposed to ultraviolet radiation within a defined spectrum. Narrowband UVB Therapy, emitting at 311–313 nm, has become the most widely used modality in modern dermatologic practice. Proposed mechanisms include T-cell apoptosis in the epidermis, downregulation of Th1 and Th17 cytokine pathways, and – in vitiligo – activation of follicular melanocytes with subsequent migration into depigmented lesions (1).
Biologics take a systemic route. These injectable medications block specific immune signaling proteins – TNF-α, IL-17, or IL-23 – to shut down the inflammatory cascade driving conditions like plaque psoriasis. Newer agents achieve PASI 90 rates above 70% in trials (3). The trade-off: ongoing prescriptions, cold-chain logistics, regular lab monitoring, and an insurance approval process that has grown increasingly adversarial. Prior authorization denial rates for biologics hit roughly 51% in 2026, with dermatology claims rejected at about three times the industry average (4).
Short-Term and Long-Term Costs
The numbers here are not subtle.
A 2026 JAMA Dermatology study – Harvard Medical School researchers simulating outcomes for 500,000 patients with moderate-to-severe psoriasis – reported mean annual total costs of $84,034 for biologics, $14,760 for office phototherapy, and $6,222 for home phototherapy (5). Out-of-pocket expenses landed at $2,000/year for biologics (often subsidized by manufacturer programs), $5,004 for office phototherapy, and $1,450 for home treatment (5).
Stretch that to a three-year window and the gap becomes stark. One analysis estimated secukinumab at $182,718 over three years, while home phototherapy totaled around $5,000 – device purchase plus occasional bulb replacement (6). A separate JAMA Dermatology analysis of 76,000+ patients showed biologic treatment cost climbing from $21,236 annually in 2007 to $47,125 in 2021. Some IL-23 inhibitors now exceed $70,000 per year (7).
A systematic review covering 34 studies and 5,123 patients confirmed the pattern: NB-UVB came in as the most cost-effective psoriasis therapy at $1,714/month per PASI 75 response. The cheapest biologic, infliximab, cost $2,076–$2,502/month for the same benchmark (8). Is phototherapy cheaper than biologics? Every published dataset says yes.
Long term cost phototherapy vs biologics matters for clinic planning too. Phototherapy equipment is a capital expense that generates reimbursable sessions over years. Biologics tie a practice to pharmaceutical pricing it cannot control. For a full picture of how reimbursement works, see our insurance coverage overview.
Effectiveness and Practical Considerations
The 2026 JAMA Dermatology simulation found biologics achieved a mean PASI reduction of 91.6%, phototherapy reached 71.1%, and a step-therapy protocol – 16 weeks of phototherapy first, then biologics only if PASI 90 wasn’t hit – delivered 95.2% with less outcome variability than either standalone option (5). That step-therapy finding deserves attention. It means starting with phototherapy and escalating as needed produces results on par with – or better than – jumping straight to biologics, at a fraction of the psoriasis treatment cost.
Phototherapy also has 40+ years of safety data behind it. No lab monitoring required. It combines safely with topicals, methotrexate, and even biologics themselves. A 2025 cohort study showed adjunctive NB-UVB restored clinical response in patients experiencing secondary failure on adalimumab (9). That kind of flexibility matters in real-world practice, especially with pediatric patients where clinicians and families are often reluctant to start immunosuppressive therapy.
Biologics remain the right call for severe, refractory psoriasis and for patients with psoriatic arthritis or major comorbidities. But a meaningful share of moderate-disease patients can reach adequate control through UV therapy cost that sits well below the biologic threshold. Around 62% of patients undergoing NB-UVB achieve at least PASI 75, and treatment courses can be repeated without the cumulative organ toxicity risks that accompany long-term systemic immunosuppression (8).
Clinic vs Home Treatment Options
Phototherapy works in both settings – and published evidence shows comparable results between office and home delivery. A 2026 meta-analysis on home NB-UVB for vitiligo confirmed it is not inferior to in-office treatment in efficacy, adverse events, or adherence (10).
For clinics, in-office phototherapy creates predictable, recurring revenue through CPT-coded sessions. It also broadens the service menu: the same equipment treats psoriasis, vitiligo, atopic dermatitis, mycosis fungoides, and other inflammatory dermatoses. Practices looking to expand services with multi-indication phototherapy gain efficiency without duplicating capital investment.
For patients, home units eliminate the two-to-three weekly clinic trips that drive many toward biologics in the first place. Research from Brigham and Women’s Hospital flagged that phototherapy facilities cluster in large cities and along US coasts, leaving suburban and rural patients underserved (5). Home devices close that gap. UVTREAT supplies professional-grade equipment for both B2B clinical use and B2C home treatment, designed to meet the protocols endorsed by AAD and BAD guidelines.
One important note: phototherapy vs biologics is not always the relevant comparison. Accurate diagnosis comes first – distinguishing psoriasis from fungal infection, for instance, changes the treatment pathway entirely.
Which Option Makes More Sense
The 2026 JAMA Dermatology data put it plainly: from the payer perspective, home phototherapy generated the highest net willingness to pay (+$11,694/patient), while biologics produced a negative net value (−$59,926/patient) (5). Step therapy achieved comparable efficacy to biologic monotherapy with lower cost and lower variability.
For clinics operating in a landscape where half of biologic prior authorizations get denied, investing in affordable phototherapy options is a practical, evidence-backed move. Phototherapy delivers clinical reliability, broad indication coverage, and financial predictability that biologics cannot match at the system level. Biologics remain essential for severe disease – but a pathway that starts with phototherapy is supported by the strongest available evidence.
Conclusion
The cost of phototherapy vs biologics is not a close contest. Annual home phototherapy costs sit under $6,500; biologics run $47,000–$84,000 depending on the agent and payer structure. Phototherapy equipment is a one-time investment for clinics; biologics are an ongoing pharmaceutical dependency. Starting treatment with phototherapy and escalating only when needed produces excellent outcomes at markedly lower cost. For both practices and patients, that is the pathway the data support.
References
- Torres AE, Lyons AB, Hamzavi IH, Lim HW. Role of phototherapy in the era of biologics. J Am Acad Dermatol. 2021;84(2):479–485.
- Elmets CA, Lim HW, Stoff B, et al. Joint AAD–NPF guidelines of care for the management and treatment of psoriasis with phototherapy. J Am Acad Dermatol. 2019;81(3):775–804.
- Egilman AC, Kesselheim AS, Avorn J, et al. Use of efficiency frontiers to align prices and clinical benefits of biologic therapies for plaque psoriasis. JAMA Dermatol. 2024;160(4):421–428.
- Medical Billers and Coders. Are dermatology biologic claims facing more denials in 2026? Published February 11, 2026.
- Kong EL, Buzney EA. Benefits and costs of biologics and phototherapy in psoriasis treatment. JAMA Dermatol. 2026;e256193.
- Mustafa SS, et al. Psoriasis treatment cost comparison: biologics versus home phototherapy. Am J Pharm Benefits. 2018;10(1):18–21.
- Rome BN, Han J, Mooney H, Kesselheim AS. Use and cost of first-line biologic medications to treat plaque psoriasis in the US. JAMA Dermatol. 2025;161(6):622–628.
- McCoy T, Natarelli N, Pan A, et al. Systematic review and estimated cost-efficacy of biologics compared with NB-UVB for moderate to severe psoriasis and atopic dermatitis. Int J Dermatol. 2023;62(8):986–999.
- Tribolet de Abreu I, et al. NB-UVB may restore adalimumab efficacy in chronic plaque psoriasis. Photochem Photobiol Sci. 2025.
The effectiveness of home-based phototherapy in vitiligo: a systematic review and meta-analysis. Photodermatol Photoimmunol Photomed. 2026.
FAQ
-
Yes, and the gap is wide. A year of home phototherapy comes in around $6,222. Three years lands near $5,000 total. Biologics sit at roughly $84,034 per year at the system level, and certain agents push past $182,000 over a three-year stretch (5, 6). No published dataset reverses that ranking.
-
It depends on the drug. Older biosimilars can be found closer to $12,000 annually, while newer IL-23 inhibitors cross $70,000 (7). By 2021 the average across all classes had reached $47,125 - and prices keep climbing. What a patient actually pays out of pocket comes down to their plan design and whatever copay program the manufacturer happens to offer that year.
-
Over four decades of clinical use say yes. Roughly 62% of psoriasis patients hit PASI 75 on NB-UVB, and courses can be repeated without the cumulative organ toxicity that limits some systemic drugs (8). Long-term protocols are backed by AAD, NPF, and BAD guidelines, and home-based treatment holds its own against in-office delivery on efficacy (2, 3, 10).
-
When phototherapy or conventional systemics haven't done the job, or when the clinical picture calls for something more aggressive - psoriatic arthritis, rapidly progressive disease, or severe comorbidities. AAD guidelines favor a stepwise approach: phototherapy first, biologics if needed (2). The 2026 JAMA Dermatology simulation confirmed this pathway reaches comparable outcomes at far lower cost (5).